HistioUK - In it Together
Our research programmes provide a beacon of hope for the many children and adults battling Histiocytosis, to ensure this research continues in these difficult times we ask you to pledge your support by making a donation today. THANK YOU.
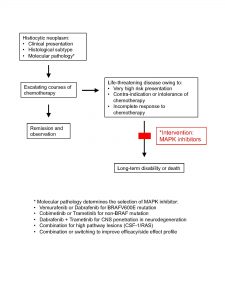
A message from some of the Clinicians & Researchers that your donation supports.